

Dental Implants in London
Happy Smiles Dental
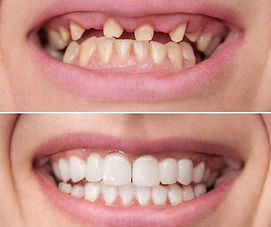
Missing Teeth?

Discover a Natural-Looking Solution with Dental Implants.
Missing one or more teeth and considering a long-lasting, natural-looking solution? Our London clinic provides premium dental implants, placed by our resident Specialist in Periodontics and Implant Dentistry.
We use premium dental implants from Straumann—a world-renowned Swiss manufacturer known for excellence and reliability. Our implants are placed with precision and care, all at very competitive prices.
Book your consultation today and take the first step toward restoring your smile with confidence.
What Is a Dental Implant?
Dental implants offer a range of benefits for those seeking a long-term solution for missing. They provide a natural look and feel, closely resembling your own teeth, which can boost your confidence.plants also help maintain jawbone health by preventing bone loss that often occurs with missing teeth.
Additionally, they make eating and speaking easier, allowing you to enjoy a full, active lifestyle without the worry of dentures slipping or discomfort.



The Procedure
Surgery Day
Your surgery day at Happy Smiles Dental is designed to reflect our commitment to personalised, comfortable care supported by advanced technology. From the moment you walk in, our warm and friendly team welcomes you into a calming, supportive environment where your comfort is our priority. If you’re feeling anxious, you can trust that our experience in caring for nervous patients ensures you’ll receive gentle, compassionate support throughout your visit.
Before we begin, we’ll go over your tailored treatment plan once more to ensure every detail has been thoroughly reviewed by our clinical team and our in-house laboratory. Using cutting-edge technology, we carry out your implant placement with precision and efficiency—all while focusing on delivering a truly pain-free experience.
Throughout the procedure, we keep you fully informed and comfortable, offering gentle sedation and continuous monitoring to help ease any worries. Our dedicated team stays by your side at every stage, making sure you feel safe, reassured, and relaxed from beginning to end.
At Happy Smiles Dental, we believe your surgery day should be smooth, calm, and confidence-inspiring. We are committed to making your transformation as comfortable and stress-free as possible—laying the foundation for a lifetime of healthy, beautiful smiles.
